What Is Facial Nerve Palsy? Understanding Causes, Symptoms, and Recovery
Facial nerve palsy is weakness or paralysis of the muscles of the face caused by damage or inflammation of the facial nerve (the 7th cranial nerve).
This nerve is responsible for much more than just facial expression. When the nerve is not working properly, different functions can be affected—often quite suddenly. The facial nerve plays a role in:
Smiling, frowning, and blinking
Closing the eye and protecting it
Tear and saliva production
Taste (front two-thirds of the tongue)
Speaking, eating and drinking
Hearing (sound volume, sound sensitivity)
What does facial nerve palsy look like?
Facial nerve palsy most commonly affects one side of the face. People may notice:
Drooping of the mouth
Difficulty closing the eye
Changes in speech or eating
Reduced facial expression
Dryness or watering of the eye
What causes facial nerve palsy?
There are many possible causes (over 50), but the most common include:
Bell’s palsy
Inflammation around the facial nerve and this pressure causes facial paralysis on the affected side. The most common cause of facial palsy.
Ramsay Hunt syndrome
Trauma or surgery
Tumours (rare)
Infection
Lyme Disease
Neurological conditions such as a Stroke, Guillain-Barre Syndrome or Facioscapulohumeral muscle dystrophy
Understanding the cause is important, as it influences recovery expectations and treatment options.
Understanding the facial nerve: structure and branches
To understand facial palsy, it helps to understand how the nerve works. The facial nerve begins in the brainstem and travels through a narrow bony canal in the skull before exiting just in front of the ear. From there, it spreads across the face like a tree.
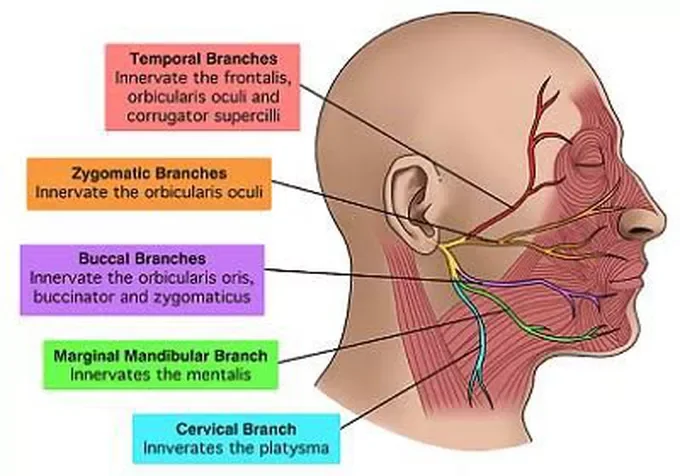
It then divides into five main branches, each responsible for different areas of facial movement:
1. Temporal branch
Controls the forehead
Raises the eyebrows
Helps with eye closure
2. Zygomatic branch
Helps close the eye
Important for blinking and eye protection
3. Buccal branch
Controls muscles of the upper lip and cheek
Important for smiling and showing teeth
4. Marginal mandibular branch
Controls the lower lip
Important for expressions like pouting or showing lower teeth
5. Cervical branch
Controls muscles in the neck
Contributes to lower facial movement
Because of this branching structure, different areas of the face can be affected differently and recovery may not happen evenly across all regions.
Understanding nerve injury: the three classifications
Not all nerve injuries are the same. The severity of injury has a big impact on recovery.
There are three main classifications:
1. First degree injury (mild injury)
The nerve is intact but not conducting signals properly
Often caused by compression or mild inflammation
Recovery: Usually good, often within weeks
2. Second degree injury (moderate injury)
The nerve fibres (axons) are damaged, but the outer structure remains intact
The nerve needs to regrow
Recovery: Takes longer, with initial recovery expected in 4 months however recovery outcome is often positive
3. Third degree injury (severe injury)
The nerve is completely disrupted
Regrowth requires intervention
Recovery: Often incomplete
Nerves regenerate slowly (around 1 mm per day) which explains why recovery can take time. As the nerve heals, signals begin to return to the muscles. However, this process is not always perfect. Some people may experience delayed return of movement, tightness or stiffness or synkinesis (unwanted linked movements, such as the eye closing when smiling). This is why recovery is not just about if movement returns—but how it returns.
The impact of facial nerve palsy on day to day life
Facial nerve palsy can affect everyday function in ways people don’t always expect:
Difficulty eating and drinking
Challenges with speech clarity
Eye irritation or dryness
Fatigue from trying to control facial movement
Changes in facial symmetry
Difficulty expressing emotions and social cues
Even simple tasks—like smiling or blinking—can require effort and concentration.
There can be a significant emotional and social impact surrounding facial nerve palsy which, at times, be underestimated. For many people, this part of the condition is just as important as the physical recovery.The face is an important factor in how we communicate and connect with others.
Facial nerve palsy is a complex condition that affects both movement and our identity. Understanding how the facial nerve works—and what happens when it is injured—can help make sense of the recovery process. With the right support and guidance, many people can make meaningful improvements—not just in movement, but in confidence and quality of life.
At The Rehab Team, our Neurological Physiotherapists provide assessment and rehabilitation for people living with facial nerve palsy.
As a mobile physiotherapy service, we provide treatment in the comfort of your own home throughout Tauranga, Mount Maunganui and Papamoa however online appointments (telehealth) are a great option for those who live outside of our region.
If you our like support, our team would be happy to discuss whether physiotherapy may help support your recovery - Here.
Want to know more?
Link to our other blog posts.